A robust and proactive accounts follow up is what we do to keep your days in A/R under the industry benchmark.
One of the common issues when performing a physician billing department assessment, or a more broad based medical practice analysis, is the lament: “Why aren’t we collecting more of our accounts receivable”.
When we ask questions about medical accounts receivable, we usually get answers like, “Oh, our AR is very low!” or, “Our AR is $XX”, with no way to tell if that’s good, bad or ugly.
One of the reasons straight answers are hard to come by is that many staff members responsible to manage accounts receivable don’t know the relevant benchmarks to use for measuring performance. So they fall back on generalities or dollar amounts with no context. No wonder physicians are skeptical and frustrated.
In fact, it’s fairly easy to monitor the overall performance of your accounts receivable efforts, and looking at these measures each month can provide an early warning of potential collection problems – and the effect on cash flow using the best practices at WPS .
Our best practice to measure and improve your AR is impressive.
We support A/R follow up to full range of payers:-
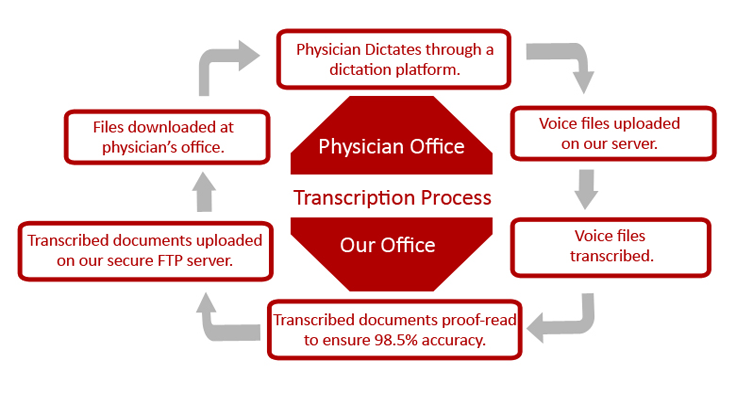
WPS offer a wide range of medical transcription services adapted for varying scales of operations from a physician’s office and clinics to multispecialty hospitals and practices, etc.
If your medical transcription needs are taken care of by us, we send all the consultation reports to the referring physicians enabling you to keep them updated about their patients' health status in time, ensuring healthy relationships between you and them, in turn generating more referrals to you.
WPS offers complete medical coding which helps in reducing payroll costs, assuring high accuracy levels, provide satisfactory results both for clients as well as their patients.
 ICD, CPT, and HCPCS coding is one of the most important tools of revenue generation. Our experienced and certified coders correctly code all the procedures and supplies along with their corresponding diagnoses by using most updated coding books and coding tools and ensure you are paid fully for all the services you provide. Our coders are also aware about the ICD 10 which will hit the Medical Billing process in October 2014 which will affect the revenue generation.
ICD, CPT, and HCPCS coding is one of the most important tools of revenue generation. Our experienced and certified coders correctly code all the procedures and supplies along with their corresponding diagnoses by using most updated coding books and coding tools and ensure you are paid fully for all the services you provide. Our coders are also aware about the ICD 10 which will hit the Medical Billing process in October 2014 which will affect the revenue generation.
One challenge that the entire healthcare industry is bound to face this year is the conversion of ICD-9 to ICD-10 coding guidelines, effective October 1, 2014.
It requires that physician practices, hospitals, health systems, payers, clearinghouses and software vendors discontinue use of the previous ICD-9 code set and adopt ICD-10 by October 1, 2014. The transition to ICD-10 is a comprehensive undertaking that impacts every facet of the billing business. It calls for significant modifications to clinical documentation, coding processes, and workflows. If it is not managed properly, the resulting productivity losses, claim denials, and impact on revenue could be devastating. At WPS we are fully prepared for this transition so that our customers are well protected from the impact of the transition.
Completely revolutionizing how healthcare information will be collected, documented and used, the ICD-10 code set provides a much more specific picture of the physician-patient encounter and plays an essential role in the practice of medicine — from how claims are processed and paid to analytics, research and quality measures.
The industry expects that ICD-10 will deliver :
It is important to remember that this transition will make practices more efficient and data more reliable — ultimately improving the quality of patient care.
The Department of Health and Human Services (HHS) mandated that, ICD-10 encompasses both diagnosis (CM) and inpatient procedure coding (PCS). The differences between the two versions are significant :

We offer comprehensive medical coding and billing services, thus helping in reducing payroll costs, assuring high accuracy levels, provide satisfactory results both for clients as well as their patients. In addition, we offer highly competitive rates to our clients for our medical billing services using the best of propriety tools in the business.
We understand that you are unique, so we offer customized services to meet your needs. We know you need attention, so our personalized services are designed to provide you designated customer service for undivided attention.
We have expertise in all major specialties such as :
WPS is dedicated to providing outstanding billing and accounts receivable services to medical practices, hospitals and ASC setup. We also serve as backbone to small, big billing companies that sub-contract to us for increased profitability.
At WPS our Medical Billing best practices will enhance the efficiency and productivity of your practice.
We follow medical billing best practices to help the healthcare organizations take their billing and collections to new heights.
We will show you that there aren’t any secrets about managing the revenue cycle – the entire process from scheduling an appointment to sending a patient statement for a final balance due. All you need is to understand how to integrate medical billing best practices into your practice. And that’s where we can help to transition your healthcare organization to a profitable center with amazing patient care.
Medical Billing Best Practice for each step :
With WPS, you know your practice is in right hands. We know what we are doing, so you are rest assured that you will see the profits of outsourcing to us. You can concentrate on the patient care.
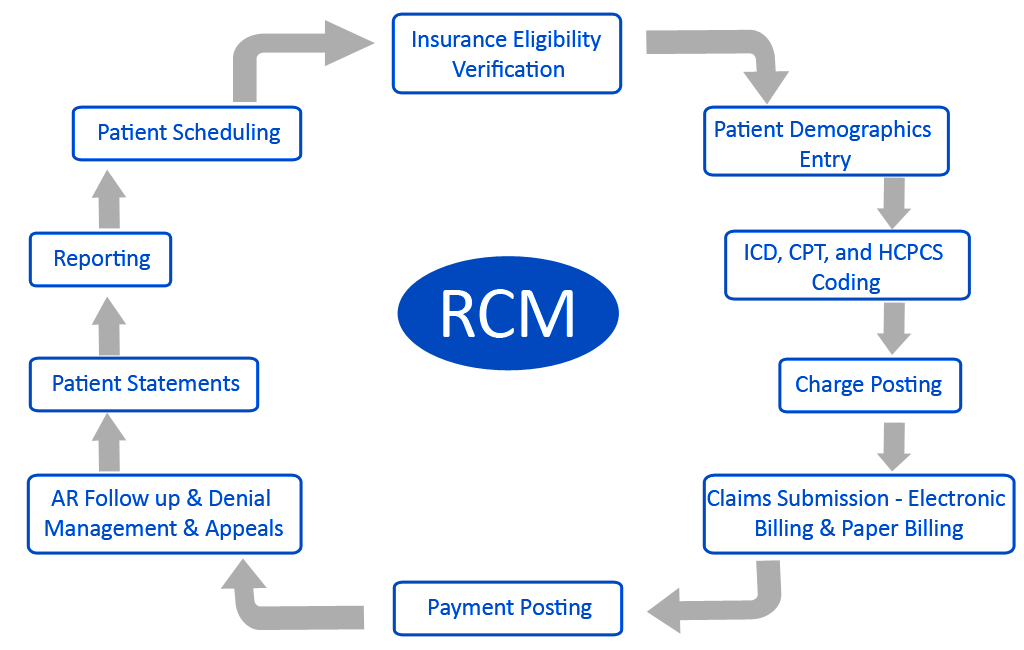
The largest value driver in healthcare BPO partnerships continues to be physician revenue cycle management. As leaders in RCM/BPO industry, WPS sets new standards in healthcare performance. Our revenue cycle model, transforms clinics to highly efficient , cost effective patient centric practice which makes the doctors more productive thus enjoying healthy and profitable medical practice.
Our robust RCM solution offers a complete set of customized services:
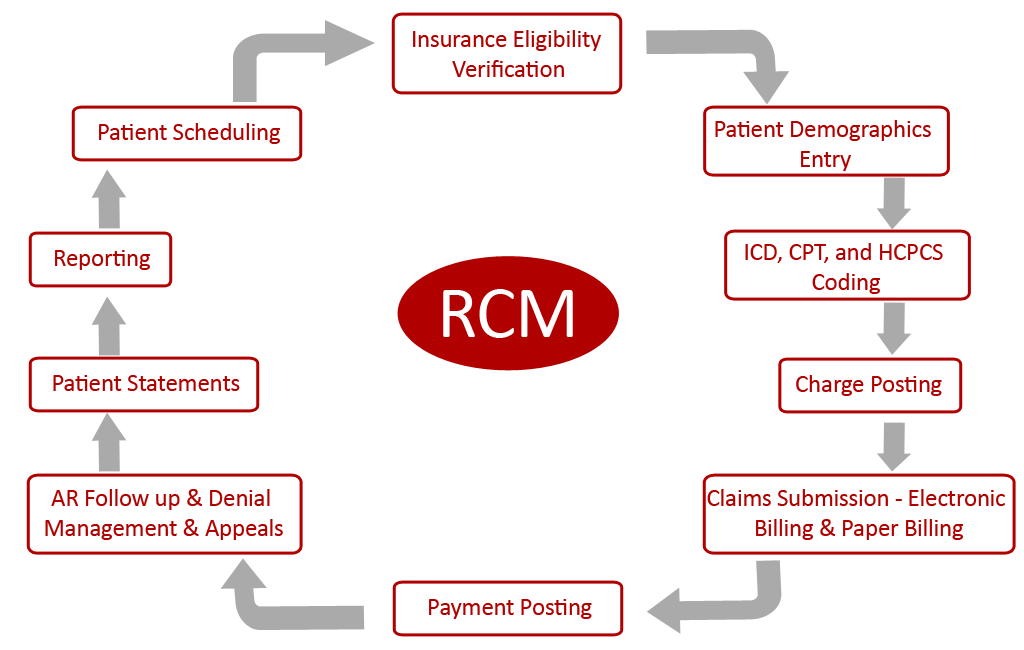
In addition, our experienced Accounts Receivable team rigorously follows all unpaid claims after each i nsurance's minimum claim adjudication period and ensures that you have least days in accounts receivable, thus optimizing your revenue cycle and increasing your cash flow.
At WPS our RCM models at WPS crosses the traditional boundaries to take your practice to new heights.